Predictable Precision Implant Placement Using Dynamic Surgical Guidance: a Five-month Follow-up
- Jan 13, 2021
- 4 min read
Updated: Jan 21, 2021
The following case was performed at the Pacific Dental Convention’s Live Surgical Stage held March 8th, 2018 in Vancouver, BC.
The patient is a healthy 58 year old male with no known allergies or medical contra-indications to dental treatment. Patient presented with a Class III malocclusion for which he received both orthodontic and oral surgery consultations; however, he was not interested in proceeding with these treatments. The patient has had extensive restorative dental treatment and has missing teeth, including number 47; extracted more than four years (note: panoramic radiograph was taken 5+ years).
Tooth number 46 had a root canal treatment that was restored with a full gold crown. The patient presented with a fistula in the buccal furcation region. Upon probing, depth was greater than 10mm and a PA of the area showed a lesion from the apical third of the mesial root up to the furcation. Clinical and radiographic findings were consistent with a root fracture.
The following treatment options were discussed with the patient:
It was also recommended to have implants placed in sites 46, 47, and 36 to allow for bilateral posterior rehabilitation and function. Five months prior to the Live Surgical Stage, tooth number 46 was atraumatically extracted.
Due to the extent of the lesion and inability to achieve primary initial implant stability, socket grafting was performed to allow for future implant placement (option 2). The socket was debrided, decorticated and grafted with a particulate allograft made up of 50/50 corticocancellous bone. The graft was overlaid with a PRF membrane which was then overlaid with a non-resorbable PTFE membrane (open-membrane technique for socket preservation and tissue development). This resulted in a band of keratinized tissue that granulated in eight weeks and covered the graft until maturation.
At the fourth month post-extraction appointment, patient returned for healing evaluation. A good zone of keratinized tissue bucco-lingually was seen with adequate tissue thickness required for biological width of final implant position apico-coronally. Real-time surgical navigation was used to perform this surgery as it offered several advantages to freehand surgery. Given both soft and hard tissue sites were developed the goal was to perform minimally invasive surgery via flapless approach. By not making an incision and raising a flap the blood supply to the ridge would be kept intact thus lessening the potential for peri-implant crestal bone loss. The lack of an incision would also mean no suturing and minimal post-op discomfort to the patient.
By using real-time surgical navigation and pre-planning the ideal implant position with the final prosthesis in mind, we are able to predictably position the implant atraumatically with proper positioning for both function and aesthetics. As well, surgical time is reduced, which is always positive for the patient. With real-time surgical navigation there are no surgical guides and irrigation is managed in the same fashion as with conventional free-hand surgery. Therefore, implant preparation is predictable and prepared in a precise manner, feeling the bone quality throughout the procedure.

In more difficult cases where critical anatomy is a concern: lingual concavity, border of the inferior alveolar nerve, incline of the mental canal, real-time surgical navigation allows the surgeon to visualize the anatomy.
During the fourth month post-extraction appointment, a CBCT scan was taken using a fiducial. The fiducial is a marker used to register the patient’s position within a 3D planning software. The planned case is used in conjunction with Inliant, a real-time surgical navigation system (the system consists of a fiducial, planning software, computer, surgical grade monitor, handpiece and cart).
Surgical accuracy is essential. While free-hand surgical osteotomies are often adequate, guided surgical osteotomies are almost always more accurate. It was elected to use a free-hand surgical guided method in order to visualize the crestal bone, interpret the apical aspects of the osteotomy and plan using 3D software. As such, the Inliant System was the free-hand surgical guided method selected for the Pacific Dental Convention’s Live Surgical Stage.
Using the Inliant System allows the clinician to see the drill’s position (large green dot in the centre of the target), angulation (smaller white circle in the middle of the large green dot) and depth (green stem seen under the target) while preparing the implant site, visualized on a monitor, all in real-time. Following the live surgical presentation, a CBCT scan was taken with the patient wearing the same Inliant fiducial used for the pre-op surgical scan and surgery. This allows for the comparison of the implant placement against the actual pre-operative 3D plan.
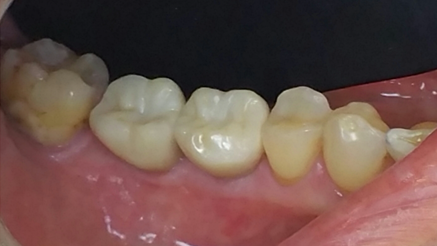
Three months after the real-time surgical navigation the patient presented for evaluation of the implants for the restorative phase. At this time the soft tissue profile looked favourable and ISQ readings, using an Osstel Unit, were taken to check the osseointegration values. ISQ values were also taken to determine if loading was possible. The relative readings were as follows: tooth #46 MB=88, DB=88 L=88 and tooth #47 MB=85, DB=86 L=85. Fixture level impressions were taken for the final prosthesis. The restorative phase was completed one month later and the patient will maintain his routine hygiene recall and implant recare protocol at our office.
Download a printable PDF


























alignersfit is your go to place for invisalign aligners that are comfortable and effective Start your journey to a perfect smile today